Physician Licensing Fees and Eligibility Requirements
- Here you will find the Physician licensing fee structure, and information on the requirements for Full, Limited, and Temporary licensing in Massachusetts: Physician Licensing Fees and Eligibility Requirements | Mass.gov
Full License Renewal Instructions
- Link here
- Please follow the Renewal Instructions to assist you in completing your renewal application.
- Specific instructions are provided for each item on the renewal application and for any additional documentation required to complete the renewal process.
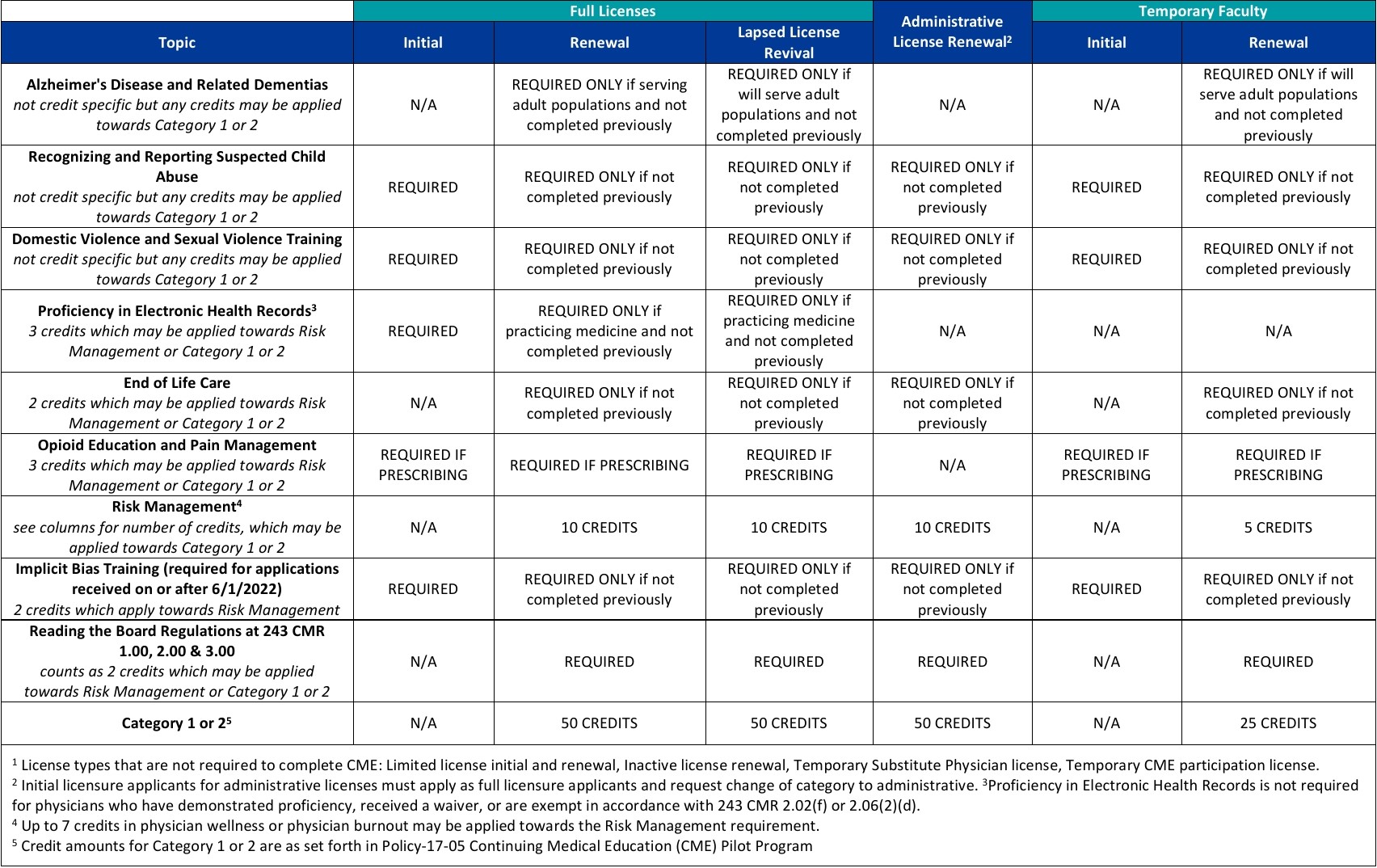
Waiver of CME Requirements
In the event that a physician is unable to complete the CME requirements by date of license renewal, a CME Waiver Request Form must be completed and submitted with the license renewal form to the Board no later than 30 days prior to the renewal date. Visit the Board's website at Board of Registration in Medicine | Mass.gov for specific details and the CME Waiver Request Form and instructions.
FAQ about the MassHealth Enrollment Requirement
- Enrollment information for MassHealth
- Link here
ONE-TIME REQUIREMENTS
Alzheimer's Disease & Related Dementias
Renewal Requirement for Alzheimer's Disease Continuing Medical Education (CME) | Mass.gov
- Renewal Requirement for Alzheimer's Disease Continuing Medical Education (CME): For Physicians who serve an adult population.
Alzheimer's Disease and Related Dementias
THE LAW - Mass. Gen. Laws chapter 112, section 2:
“The board shall require that any continuing education requirements necessary for the renewal of a physician's certificate of registration include the 1–time completion of a course of training and education on the diagnosis, treatment and care of patients with cognitive impairments, including, but not limited to, Alzheimer's disease and dementia; provided, however, that this course requirement shall only apply to physicians who serve adult populations.”
St. 2018, c. 220
BASIC FACTS
- This is a One-time requirement.
- The requirement is for a minimum of 1.00 CME credit (1 hour)
- This is required for renewing licensees only, not initial or limited licensees.Courses taken in past education or training can satisfy the requirement.
- The requirement only applies to physicians who serve adult populations.
- The Board of Medicine has waived this requirement until Dec. 31, 2020.
- You must complete this requirement by Nov. 7, 2022.
End-of-life Issues
End-of-life Care refers to the medical and ethical issues surrounding the end of a patient's life. End-of-life issues include the type and extent of medical care, services, treatments, medications and other options that may be available to the patient. End-of-life care includes palliative care as defined by 105 CMR 130.1900: Definitions Applicable to 105 CMR 130.1901.
130.1901: Provision of Information on Palliative Care and End-of-life Options
(A) Each hospital shall distribute to appropriate patients in its care, directly or through professionally qualified individuals, culturally and linguistically suitable information regarding
the availability of palliative care and end-of-life options. This obligation shall be fulfilled by providing the patient with:
(1) A Department-issued informational pamphlet; or
(2) A similar informational pamphlet that meets the specifications in 105 CMR 130.1901(B).
(B) At a minimum, the informational pamphlet shall include:
(1) A definition and explanation of advanced care planning, palliative care services and hospice services; and
(2) All other requirements defined in guidelines of the Department.
(C) Each hospital shall provide its attending health care practitioners the information in 105 CMR 130.1901(A) for distribution to appropriate patients in a timely manner.
(D) Each hospital shall have a policy to guide its attending health care practitioners for identifying appropriate patients and ensuring that they receive an informational pamphlet. Such policies shall be made available to the Department upon request.
(E) Each hospital shall inform all physicians and nurse practitioners providing care within or on behalf of the facility of the requirements of M.G.L. c. 111, § 227(c) to offer to provide end-oflife counseling to patients with a terminal illness or condition.
(F) Where the patient lacks capacity to reasonably understand and make informed decisions, the information in 105 CMR 130.1901(A) shall be provided to the person with legal authority to make health care decisions for that patient.
(G) The hospital shall make available to the Department proof that it is in compliance with 105 CMR 130.1901(A) and (C) through (E) upon request or at the time of inspection.
Proficiency in Electronic Health Records
Demonstrating proficiency in EHR is a prerequisite to medical licensure in Massachusetts – One-time requirement
Physicians, Renewing Licensees and Lapsed Licensees must demonstrate proficiency in the use of EHR in one of the following ways:
- Participation in a Meaningful Use program as an eligible professional; OR
- Employment with, credentialed to provide patient care at, or in a contractual agreement with an eligible hospital or critical care access hospital with a CMS certified meaningful use program;
- Participation as either a Participant or Authorized User in the Massachusetts Health Information Highway, “Mass HIway” OR
- Completion of three hours of a Category 1 EHR-related Continuing Professional Development (CPD) course that discusses, at a minimum, the Core and Menu Objectives and the Clinical Quality Measures for Meaningful Use. The three EHR credits may be used toward the required 10 risk management CPD credits.
Reporting Suspected Child Abuse and Neglect
Child Abuse and Neglect Training means the education and training to recognize and report suspected child abuse or neglect required by M.G.L. c. 119, § 51A(k).
Recognize and Report Suspected Child Abuse or Neglect - One-time Requirement
Physicians renewing their MA medical license must also demonstrate competence in the following area. This is NOT an accredited CME/CPD requirement.
M.G.L. c. 119, §51A(k) required all mandated reporters (including physicians), professionally licensed by the Commonwealth, to complete training to recognize and report suspected child abuse or neglect.
Physicians may comply with the training requirement through:
- Receiving training in child abuse or neglect assessment in medical school education or postgraduate training;
- Completion of a hospital sponsored training program in recognizing the signs of child abuse and neglect;
- Completion of continuing professional development (formerly known as continuing medical education credits) in identifying and reporting child abuse and neglect;
- Completion of an on-line training program (i.e., The Middlesex Children’s Advocacy Center’s program “51A Online Mandated Reporter Training: Recognizing and Reporting Child Abuse, Neglect, and Exploitation” www.middlesexcac.org/51A-reporter-training); or
- Completion of a specialized certification (i.e., Child Abuse Pediatrics).
Full license applicants must complete the requirement for training prior to submission of an application to the Board. This is a one-time requirement.
Domestic Violence and Sexual Violence Training
Domestic Violence and Sexual Violence Training – One-time requirement
Per Chapter 260 of the Acts of 2014, An Act Relative to Domestic Violence, the Board of Registration in Medicine and other health profession boards are required to develop and administer licensing standards that include education and training on domestic violence and sexual violence. This online course meets this requirement: Sexual Assault and Domestic Violence Continuing Education for Massachusetts Clinicians. The Department of Public Health has also developed an e-Learning tool that can be accessed from the DPH’s DVSV Integration Initiatives webpage: https://www.mass.gov/service-details/domestic-and-sexual-violence-integration-initiatives Only a DPH-approved course can fulfill the requirement. Training for Licensed Professionals to Meet Chapter 260 Requirements (chapter260training.org)
Implicit Bias in Health Care
The Board of Registration in Medicine (BORIM) has, as part of its mission, the goals of ensuring that physicians and the health care institutions in which they practice provide to their patients a high standard of care, and supporting an environment that maximizes the high quality of health care for all people in Massachusetts. BORIM recognizes the importance of eliminating racial and ethnic inequities that lead to health disparities in Massachusetts. Implicit bias among health care providers is one factor that perpetuates these disparities. BORIM adopts this policy to address implicit bias among healthcare providers in Massachusetts, beginning with physicians.
Beginning June 1, 2022, BORIM will require that applicants for initial physician licensure and licensees renewing physician licensure complete a continuing medical education requirement of 2.00 credits on the topic of implicit bias in healthcare. The 2.00 credits may be applied towards a physician’s biennially required 10 hours of risk management credits pursuant to 243 CMR 2.06(a)3.
Continuing Requirements – every two years
Opioids and Pain Management
Pain Management Training means the education and training required by M.G.L. c. 94C, § 18(e). Such training shall include, but not be limited to, education in opioids and other pain-relieving medications, training in effective pain management, training in how to identify patients at high risk for substance abuse, and training on how to counsel patients on the side effects and addictive natures of prescription medicines and their proper storage and disposal. Practitioners who prescribe controlled substances, except veterinarians, shall be required, as a prerequisite to obtaining or renewing their professional licenses, to complete appropriate training relative to: (i) effective pain management; (ii) the risks of abuse and addiction associated with opioid medication; (iii) identification of patients at risk for substance use disorders; (iv) counseling patients about the side effects, addictive nature and proper storage and disposal of prescription medications; (v) appropriate prescription quantities for prescription medications that have an increased risk of abuse; and (vi) opioid antagonists, overdose prevention treatments and instances in which a patient may be advised on both the use of and ways to access opioid antagonists and overdose prevention treatments. The boards of registration for each professional license that requires this training shall develop the standards for appropriate training programs. Mass. General Laws c.94C § 18 | Mass.gov Applicants who prescribe controlled substances shall, as a prerequisite to obtaining or renewing a medical license, complete appropriate Pain Management Training and opioid education, according to M.G.L. c. 94C, § 18 and 243 CMR 2.00. Pain Management Training shall consist of at least three credits of Board-approved continuing medical education and may be used toward the required ten credits of risk management training. 243 CMR 2 (mass.gov)
Risk Management Study
Risk Management CME means instruction in medical malpractice prevention, such as risk identification, patient safety, and medical error prevention. Risk management studies may include education in any of the following areas: medical ethics, quality assurance, medical-legal issues, patient relations, electronic health record education, end-of-life care, physician burnout, utilization review that directly relates to quality assurance, and aspects of practice management. Physicians may report up to 7 CME credits for content in the area of physician burnout towards the 10 required risk management credits. 243 CMR 2 (mass.gov)
Reading the Board’s Regulations, 243 CMR 1-5
Physicians must spend a minimum of 2 hours per licensing cycle studying the Board of Registration in Medicine Regulations 243 CMR 1.00-5.00. Credit may be earned in Category 2 or, when appropriate, in Category 1.

 Facebook
Facebook X
X LinkedIn
LinkedIn Forward
Forward